|
Louisiana's Oschner's Healthcare is taking patient-centric medicine one step further. They have become the first healthcare system to integrate data from Apple HealthKit directly into the EMR without need for a middleman. This represents a significant step into total healthcare continuum, and the opportunity for true lifestyle counseling. For example, the AHA recommended guidelines for physical fitness are 150 minutes of exercise a week. Simply asking a patient if they are getting that amount can lead to a highly inaccurate picture of patient health. Relying on patient to report tracking or asking office staff to check and input is likely a futile task. But being able to pull up charts and reports automatically generated in an integrated system could make a fruitful conversation around health, exercise and management of diabetes, blood pressure and cholesterol a breeze for physicians in an office visit. Lifestyle counseling, in addition to pharmacologic management, is an important piece of overall patient health for many prevalent chronic common adult-onset diseases.
0 Comments
Merry Christmas and a Healthy Happy New Year!
New Year resolutions: Get more exercise. Fortunately my new FitBit Charge HR will help with that! I love this device. A long jog on Christmas Day (thank you warm weather) let me try this out. I've upgraded from the FitBit Flex, which I've had for 15 months, and wore everyday. But I really wanted to count my steps and my heart rate, so this was a great choice! A recent medscape article that went into the depth about the diagnostic differences between chronic fatigue and fibromyalgia, reminded me about how both of these diseases can also have "brain fog" as a cognitive issue. Not being able to think clearly when at the doctor's office due to your healthcare condition can make it even harder to explain exactly how you are feeling.
An important point of diagnosis is the differences in severity between fatigue and pain.Directly quoting the article:"The difference between chronic fatigue syndrome and fibromyalgia is the intensity of fatigue and pain. Chronic fatigue syndrome involves severe fatigue and mild pain; fibromyalgia involves severe pain and mild fatigue. Also, fibromyalgia is accompanied by tenderness in multiple areas of the body." Of course if you are only suffering from one, how do you know how to compare, as a patient? It's not easy to communicate intensity and severity of symptoms to your physician, as these things can be subjective, based on your own personal experience. One rule of thumb I like to tell people about communicating severity is that:If you are experiencing a level 10 severity (the highest level, most severe), you would be thinking of going to the emergency room if it were to persist for more than 20 minutes; you would have loss of function; you would feel like cutting off the affected body part to relieve the symptom. A severe pain or fatigue would be slightly less than that, but would definitely impact function and you would be seeking medical treatment for the symptom. On a scale of one to 10, you would report a severe pain or fatigue as a level 7, 8 or 9. So ask yourself, which is worse- the pain, or the fatigue? And then quantify both on the scale of 1-10, and communicate it to your healthcare provider in that way. If you or a loved one is struggling with either of these issues, II hope this is helpful! <3 http://reference.medscape.com/viewarticle/842828 According to USA.gov, quitting smoking is one of the top 10 New Year’s Resolutions, and for good reasons. Even if your primary motivation is health, there is also a financial motivation to quitting smoking. Everyone knows the price of cigarettes is climbing, but if you are a smoker using the Healthcare Marketplace to get your healthcare insurance, you may soon be facing an even bigger financial hurdle.
In most states (New Jersey, Massachusetts, Vermont, Rhode Island and District of Columbia are among the exempt), it is legal to charge smokers more for healthcare and life insurance. This is where it gets interesting. When the Affordable Care Act was put into place, two provisions were made. One was that older plan participants could be charged 3 times more for health insurance than younger participants. The other was that smokers could be charged 1.5 times more for health insurance than non-smokers. But there was a fault error that no one could be charged more than 3 times what the least expensive participant is paying. So it became impossible for older smokers to be charged the full amount- this was referred to as the “smoker’s glitch.” However, this glitch in the computer system is being fixed in 2015, so if you are an older smoker, and using the healthcare marketplace for insurance, you should seriously consider quitting, as your rates will rise quite a bit. If your insurance company is aware that you smoke, enlisting your doctor’s help for smoking succession and reporting success at the end of 8 or 12 weeks can help save you money. Use online resources like those found at http://smokefree.gov/. Before you start, call both your health insurance company and your life insurance company, tell them if your plans, and find out exactly what they need for you to qualify as a non-smoker. Also, don’t expect to see an immediate drop in rates. For life insurance, it make take as long as two years certified tobacco-free before rates begin to drop. You may also want to find out exactly what they include or exclude as a tobacco product. Find out how they monitor. Some companies use the honor system, some companies require blood tests for nicotine, or physical exam by a physician. For example, increased rates may apply to only cigarettes for some companies. Other tobacco products, like chewing tobacco, cigars, and e-cigarettes (vaping) are exempt. This does not mean these are without health risks, so don’t be fooled. Do your research and discuss with your doctor if you plan to switch.  There is a phenomenon called “white coat hypertension” in which a person will have high blood pressure only when at a doctor’s office. This can lead to a person being treated with antihypertensive medication when they really don’t need to be. It shows the power of the body to react to anxiety.1 Part of this is rooted in a the fact that long ago, when our ancestors were scared or thought they were in danger, a part of their brain would jump into action and trigger their “freeze, flight, fright, or fight” reaction.2 They had “no time to think”, and could flee to safety or strike out at an enemy in time to protect themselves. It was the key to their survival in the dangerous world. But now, unfortunately, this response can get activated during times when we really aren’t in mortal danger, but simply anxious. And being worried can make it difficult for the complex thinking part of our brains, the prefrontal cortex, to do its job. Many people can get nervous at the doctor’s office and you may be so worried about your illness being something serious, or so uncomfortable sitting on the exam table in the that thin little paper gown, that you find it hard to remember all the symptoms you wanted to tell your physician. You may forget what instructions you are being given, and your “flight” instinct may kick in, leaving you only wishing the appointment was over and you could get dressed and leave. These types of reactions only adds to the difficulty you face during your appointment, particularly because with today’s current healthcare climate, he or she may be under a time crunch, dealing with electronic medical record inputting, and facing his or her own stressors, causing suboptimal communication. To help combat your anxiety, take a few minutes to prepare for your appointment ahead of time. Make sure you list all of your symptoms, when they first occurred and if there is a pattern to them. Write down any questions you have for your doctor ahead of time and be sure to write down any instructions your doctor gives you to help you remember after you leave the office. Ask your doctor if he or she has any reliable sources of information on the internet that they might recommend for your condition as well! Abir-Khalil S, et al. Prevalence and predictors of white-coat hypertension in a large database of ambulatory blood pressure monitoring. East Mediterr Health J. 2009;15(2):400-7. Bracha, H., Ralston, T. C., Matsukawa, J. M., Matsunaga, S., Williams, A. E., & Bracha, A. S. (2004). Does “fight or flight” need updating?Psychosomatics, 45, 448-449. 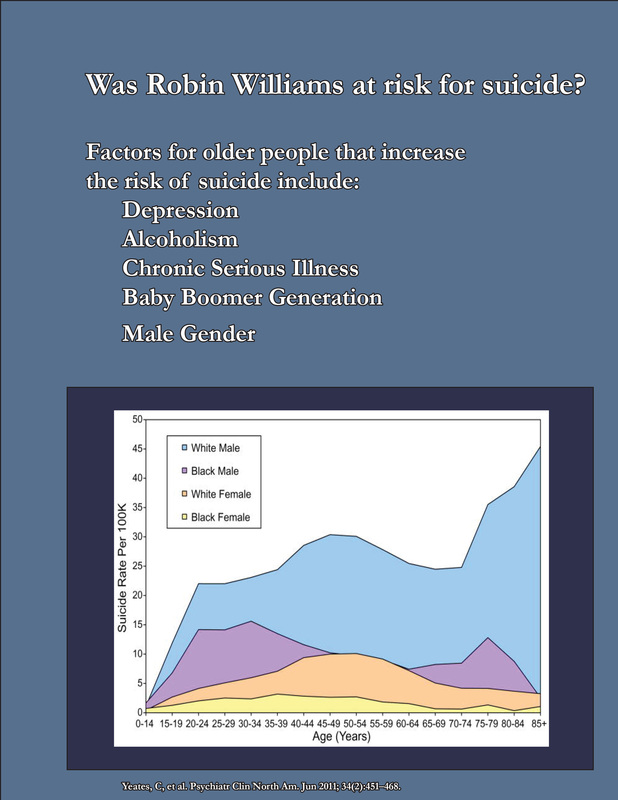 I I admit, when I heard about Robin Williams, I was shocked. Based on the reactions on social media, I was not alone. Suicide (also called intentional self-harm) the number 10 leading cause of death in the US according to the Center for Disease Control.1 Much of the material for suicide and suicide prevention focuses on adolescents and young people, and for good reason. It is the second and third leading cause of death among young people, aged 15 to 34 years, surpassed only by accidental injury. And for every suicide completion, there are many more adolescents that attempt suicide. The prevalence of suicidal thoughts, suicide planning, and suicide attempts is significantly higher among young adults aged 18-29 years. By the time a person reaches 55 to 64 years, suicide has dropped to the eighth leading cause of death. Perhaps that is why we were all so shocked. But should we have been? Buried deep within the data of suicide statistics is a terrible secret. While the above focuses on young people, the truth is this: Suicide rates at 36 per one hundred thousand, are the highest among men aged 75 years or older,2 even greater than young men (see chart below)2. Put another way, if you know about three thousand people over the age of 74, either in person, or online, or as a celebrity, you have a very good chance of knowing someone who will commit suicide as an older adult. Robin Williams was a bit younger than this group of adults at 63 years of age, but the generation of “baby boomers” has had a proportionally higher suicide rate compared to the generations before and after.2 It was known that Mr. Williams was suffering from Major Depressive Disorder, an illness commonly found among post-mortem examinations in suicide completers.2 Other neurological disorders or mental illnesses associated with suicide completion include bipolar, psychotic disorders, ADHD, and schizophrenia, as well as anxiety.2 Reports also have been made that Mr. Williams was in the early stages of Parkinson’s disease, a chronic, progressive debilitating disease. Dr. Juurlink et al, reported in the Archives of Internal Medicine, that risk of suicide in patients 65 and older with illness is particularly high for those who have recently visited a doctor and/or had multiple illnesses.3 In addition, severe pain in particular, is a much greater risk factor for men than women, according to the Juurlink study (Odds ration of 9.9 vs. 3.3).3 Mr. Williams had open-heart surgery several years ago, and heart disease is heavily linked to depression in and of itself.4 The disparity between genders begs the question of what role masculinity and traditional gender roles play in suicide risk in older men. Some studies have shown that indeed, the traditional gender roles that position men as “the strong and silent type” increase the risk of suicide in elderly men (it is interestingly, somewhat different for younger men).5,6 This may be aggravated with the tendency for males to abuse alcohol as a way of coping with stress, as many suicide completers are found with alcohol in their system (other drugs noted at high prevalence include acetaminophen, opioids and antidepressants).7 Also present is the tendency to not discuss depression, so that even those closest to the man at risk may not be aware.8 Though it’s hard to imagine a man who had one of his most successful movies dressing up as a woman, to be struggling with masculinity issues, it is well-known that Mr. Williams had trouble with alcohol use. Indeed all these factors put Robin Williams at risk of becoming another suicide statistics. Of what happened in those final, fateful moments, we may never know. “Failures plagued me. Things I had omitted or ignored, neglected. What I should have given and hadn’t. I felt the biting pang of every unfulfillment.” ― Richard Matheson, What Dreams May Come 1. http://www.cdc.gov/violenceprevention/pdf/Suicide-DataSheet-a.pdf 2. Yeates, C, et al. Psychiatr Clin North Am. Jun 2011; 34(2):451–468. 3. Juurlink DN, et al. Arch Intern Med. 2004 Jun 14;164(11):1179-84. 4. Su, S, et al. Psychosom Med. 2009 Feb;71(2):152-8. 5. Hunt, K, et al. Soc Psychiatry Psychiatr Epidemiol. 2006 Aug;41(8):641-7. Epub 2006 May 26. 6. Möller-Leimkühler AM. Eur Arch Psychiatry Clin Neurosci. 2003 Feb;253(1):1-8. 7. Jones, AW. J Forensic Leg Med. 2013 Oct;20(7):842-7. 8. Brownhill S, et al. Aust N Z J Psychiatry. 2005 Oct;39(10):921-31. There are big changes going on as far as the merger of healthcare and technology are concerned. We are now able to have more personalized monitoring of our human condition than ever before. Remember the little tricorder that Bones carried around with him in Star Trek (the original series)? Well, our smartphones can basically become that for us. Isn't that awesome?
Or is it? Bones was a licensed medical professional. He knew what to do with that information. With the advent of Google Fit and Apple Healthkit, we will have access to not just our steps taken and our heart rate, but possibly our blood sugar, our blood cholesterol, and our blood pressure. FDA regulations are such that if a device is used for diagnosis or treatment of a medical condition, it is deemed a medical device and is subject to FDA approval. Approval process of a medical device is a lengthy and expensive one, similar to that for pharmaceutical medicines. An example of this type of device would be iBGSTAR, a small glucose meter that attaches to a smartphone and software that reads glucose. A company I worked for was involved in the production and approval of this product as a medical device. Apple approached the FDA and wanted guidance for how their software was going to be perceived by the FDA. The response they got from the FDA was that their product differed from iBGSTAR because it was expected to be used by “healthy” people, not diabetics. Therefore it would not be a medical device. “The current mobile medical app guidance indicates that FDA does not view apps that are purely educational or informational as medical devices. Apps that actively measure something are considered diagnostic. For instance, a glucometer would be considered diagnostic because it measures blood sugar; it would not be considered merely information although it “informs” the user of the blood sugar level. The display screen of the glucometer would not be regulated, as it only receives the data and shows it. The software that does the measuring is the part that is regulated. FDA will regulated based on the intended use of a device. Using the glucometer example, the glucometer may be unregulated if the intent is for a user to follow their blood sugar for the purposes of better nutrition. If the glucometer is marketed for diabetics, however, it would more likely be regulated as a medical device. FDA looks at how devices are actually used” http://9to5mac.com/2014/06/09/fda-details-high-level-meeting-with-apple-moral-obligation-to-do-more-with-health-innovative-sensors/ But herein lies the rub in the reasoning of the two parties: Based on data from the CDC, a large number of people are in for quite a shock.
Then what happens? According to regulation and law, as non-medical devices, Apple Healthkit and Google Fit are not allowed to diagnose and treat. The consumer is left in a gray zone. They are given potentially life-saving information without any support. A diabetic has different blood pressure targets than a person with normal glucose. Will the devices be legally able to adjust for that? They are at risk for neuropathy and amputation and diabetic ketoacidosis. Does the device monitor for those things as well? I have not seen this scenario addressed at all in any of the briefings on these devices and I am very interested to know how these manufacturers intended to resolve these questions. There is a great potential here for early intervention, increased adherence, and education. But the lines for diagnosis and treatment by licensed medical professionals need to be maintained. I see more discussion with the FDA needed as technology and healthcare forges where no app has gone before. http://www.opptrends.com/2014/06/google-inc-goog-might-enter-health-data-space-with-google-fit/ http://www.forbes.com/sites/parmyolson/2014/06/12/exclusive-google-to-launch-health-service-google-fit-at-developers-conference/ http://www.wired.com/2014/03/apple-healthbook-is-just-the-beginning/ http://www.cdc.gov/cdcgrandrounds/pdf/gr_mh_all_final_feb28.pdf http://www.cdc.gov/nchs/data/databriefs/db107.pdf http://www.diabetesmine.com/2011/12/newsflash-fda-approves-the-ibgstar-meter-for-iphoneipod-touch.html http://9to5mac.com/2014/06/09/fda-details-high-level-meeting-with-apple-moral-obligation-to-do-more-with-health-innovative-sensors/ Photo attribution http://commons.wikimedia.org/wiki/File:DeForest_Kelley,_Dr._McCoy,_Star_Trek.jpg#mediaviewer/File:DeForest_Kelley,_Dr._McCoy,_Star_Trek.jpg *Dr. Robot says take 2 aspirin and email me in the morning*
Will artificial intelligence replace your primary physician in the future? Look at the current healthcare crises. Due in part to changes enacted by the Affordable Care Act (ACA), there will be a need for an additional 52,000 primary care physicians doctors (nearly a quarter) by 2025. The mandate of Electronic Health Records (HER) makes your health history accessible digitally, so personalizing diagnosis and treatment should be possible. Enter “Modernizing Medicine” a so-called web-based repository of medical information. It is basically data mining from patients and doctors mined and if you enter what you are looking for it spits out recommendations. Think “Trip Advisor” for medical treatment. Also, revealed at ASCO this week was an MD Anderson program, based on the WATSON platform that suggested standard-of-care diagnosis for cancer patient cases and was correct about 80% of the time. This system was named "Oncology Expert Advisor". Although I am excited by the prospects of combining the information on EHR with large-scale data mining to get personalized care for patients (let’s face it, it sounds uber-cool on paper), my 20 years experience in Pharma and regulatory is having some questions about the use of this program. Classically, recommendations are made by consensus groups of well-respected, highly experienced “key-opinion leaders” in a specialty field. They come together for about a week, present, debate, look at all the evidence for use of products in a disease state, and then publish a “consensus paper”, which is then, in turn, reviewed by a panel of peers, critiqued and sent back and forth until it is finally published. This process is renewed every few years to keep recommendations fresh. Evidence for this is generally that available in peer-review literature, graded A-D, based on large-scale clinical trials to case reports. The recommendations are produced as algorithms or consensus guidelines, which the doctor has an opportunity to follow and choose based on their patient’s individual profile. The choice is always, and should always, be left up to the licensed medical professional. Comparing the classical method to this new database: one is based on evidence-based medicine, thoughtful debate by knowledgeable men, peer-review and a tried-and-true process; the other, is a handful of single case reports gathered together and run through a program on the computer to pick the “winner.” I will say that for those diseases that don’t currently have consensus papers for treatment, however, this may be useful for helping a physician find a possible treatment, such as their example. This new method is not currently being regulated by the FDA. This also confuses me, as when I work with my Pharma clients to develop tools (websites, apps, sliders, booklets) for physicians, I am very careful NOT to tread on the diagnosis and treatment line, as I know the regulatory is very strict in that regard. I see this program as being very blurry on this treatment recommendation line. I am very interested to see how far these type of programs are taken before the FDA steps in and begins to regulate them and demand references and consensus guidelines to be used as part of the programming. http://am.asco.org/ibm%E2%80%99s-watson-based-oncology-computing-system-recommends-treatment-high-accuracy http://www.wired.com/2014/06/ai-healthcare/ By now you may have heard about Truvada. The headlines scream about the pill that will prevent HIV. Our children will never have to face a world of AIDs the way we did. This is the answer. But to look deeper behind the truth of Truvada, you will see that there is a host of issues facing this “miracle drug.” The first is who should take Truvada?
For some, it is an easy choice. If your partner has HIV and you don’t, this pill should be considered. Also, the pill has been quickly embraced by the gay porn industry, and for some injection drug users. Yet it certainly isn’t appropriate for the entire sexually active population to take this pill, as it is cost prohibitive, and no medicine is without side effects. Truvada comes with a black box warning for those with unknown HIV status, and small risk of renal impairment. As for that unknown HIV status, the CDC states that of the 1.1 million people living in the US with HIV, 1 in 8 are unaware that they are even infected.http://www.cdc.gov/hiv/statistics/basics/ataglance.html. So from this we can conclude there is a large number of people who don’t even realize they are at risk for getting HIV. It would be difficult to identify people who might benefit from Truvada if they aren’t even getting tested. For others, there is a matter of adherence. Medication Adherence by definition is the patient’s ability to do what the provider’s recommends as far as respect to timing, dosage, and frequency of medication-taking during the prescribed length of time. As you can see, this is a complicated set of instructions, which can be thrown off by any number of life events. Fortunately dosing with Truvada is simple, once daily, with or without food. Adherence is a tough pill to swallow, so to speak. According to the CDC, up to 1/3 of patients never fill prescriptions in the first place. If a person were to go on Truvada, we could expect their resolve would lessen after about 6 months; 25% to 50% discontinue therapy by one year.http://www.cdc.gov/primarycare/materials/medication/docs/medication-adherence-01ccd.pdf And what of cost? HIV does not discriminate, it infects folks of any socioeconomic class, and prevention drugs of this type are not often covered by health insurance, though Medicaid and some insurance companies are starting to foot the bill; Gilead offers a reimbursement program if your insurance company is one that does not cover the $1,000 a month cost. Truvada, for those who know they are at risk and will remain adherent and experience no side effects, is a wonderful advance. But there still needs to be an eye on overall STD prevention, HIV testing, and vaccine development.  Credit: Alex E. Proimos on Flickr, under Creative Commons (CC BY 2.0). Stress and Physician Workload Credit: Alex E. Proimos on Flickr, under Creative Commons (CC BY 2.0). Stress and Physician Workload *At least 1 in 20 US adults are misdiagnosed* According to a recently published study in BMJ Quality and Safety. Unlike previous studies that reviewed only malpractice cases, they actually reviewed patient charts for multiple visits (a more realistic snapshot) and saw who had been diagnosed improperly the first time and had to return again and again to get proper treatment. The study authors admit that even this method underestimates patients who are lost to follow-up or who just give up or turn to alternative treatments. The authors also conclude roughly half of these misdiagnosis lead to harmful outcomes for the patients. http://qualitysafety.bmj.com/content/early/2014/04/04/bmjqs-2013-002627.abstract *Physician salary is still largely based on number of patients they see per day* In a survey released by Medscape of physicians, almost half (47%) of the physicians asked, stated that they see between 76 and 200 patients a week. Most physicians spend less than 40 hours a week seeing patients (other time is spent on administrative duties). And guess which type of doctor is the most overloaded? The gatekeeper for the specialists and the pathway to diagnosis! (see study above) According to the CDC, the annual visit load for your primary care physician is 30% higher than for specialists. This is in part, due to physician shortages across the US, particularly in primary care. In spite of payment reforms related to the Affordable Care Act, how much money a practice makes is still generated by how many patients a physician sees per hour! Medicare is known to have lowered fees, private insurers are also paying less, particularly to small practices without any strong influence. The Medscape survey has found that this has led to a drop in job satisfaction for physcians, not surprisingly. http://www.medscape.com/features/slideshow/compensation/2014/public/overview#18 If misdiagnosis and 5-minute office visits become the status quo, treatment is delayed, patient out-of-pocket costs skyrocket, inappropriate treatment is given, medications that actually could help are not taken, and non-pharmaceutical options are not explored. Both the patient and the physician are feeling the frustration of this process. |
Dr. Diane CleverleySubscribe to the RSS feed by adding an RSS reader, like Feedly, NewsBlur, or OldReader. For more info watch this video: http://www.youtube.com/watch?v=0klgLsSxGsU Archives
October 2017
Categories
All
|




 RSS Feed
RSS Feed
